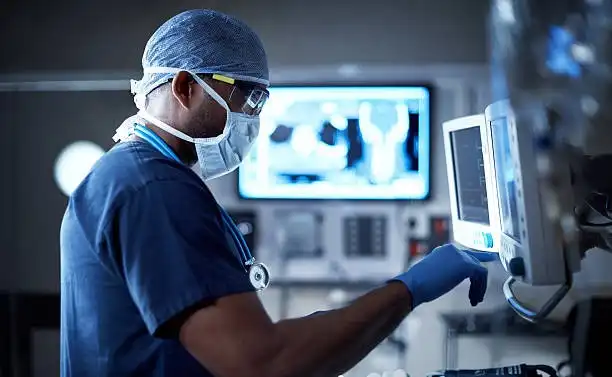
If your symptoms indicate active bleeding in the esophagus, your doctor may do what’s called an esophagogastroduodenoscopy (EGD).
Mueller-Weiss Syndrome: What to Know
Mueller-Weiss syndrome is a rare condition that causes severe arch pain on the inside of your mid- and hindfoot. It’s mostly found in people ages 40-60, and it’s much more common in women. It’s a progressive disease, meaning it gets worse over time, and it usually affects both of your feet. It causes flatfoot, which happens when your arch collapses. It can also cause your feet to be disfigured or bent out of shape.
What Causes Mueller-Weiss Syndrome?
Experts don’t know its exact cause. But they think it may be caused by things like:
- A forceful squeeze or compression on the cluster of bones in your midfoot (known as the lesser tarsus)
- A birth defect (congenital)
- The loss of blood supply to your navicular bone (ischemia)
Your navicular bone is a half-moon or boat-shaped bone in the middle of your foot. If it suddenly loses its blood supply, your bone tissue starts to die, which then causes your joint to erode and your bone to collapse over time.
Your navicular bone also happens to be the last bone to fully form (known as ossification) in your foot during childhood. If this bone was slow to form, you might be at risk for Mueller-Weiss syndrome. Research also suggests you might be at higher risk if you’re obese or overweight.
What Are the Symptoms of Mueller-Weiss Syndrome?
- Severe midfoot pain
- Foot swelling
- Tenderness on top of your feet
- Arch pain
- Trouble walking
- Your navicular bone becomes comma or hourglass shaped.
But it might take months or years before you notice any symptoms.
How Is It Diagnosed?
Because Mueller-Weiss syndrome is uncommon, it’s often under- or misdiagnosed. That’s because doctors might be slow to identify flatfoot issues. If you have foot pain, especially in your arch or around your midfoot, let your doctor know.
They may refer you to a podiatrist (foot and ankle expert) or an orthopedist (doctor who specializes in bones). They’ll take your detailed medical history and examine your feet.
They may run a few imaging tests on both of your feet. Those may include:
This will help them get a clear picture of what’s going on. Based on the amount of tissue death and erosion you may have in your navicular bone and its surrounding area, they’ll stage your condition and symptoms as mild (stage 1), moderate (stage 2-3), or severe (stage 4-5).
What Are the Treatment Options?
For now, there isn’t one best treatment for Mueller-Weiss syndrome. If your condition and symptoms are in the early stages, your doctor may prescribe nonsurgical therapies to help improve your quality of life.
These may include:
- Anti-inflammatory medications (NSAIDs)
- Braces that cover and support your foot and ankle (ankle-foot orthosis)
- A temporary foot cast to stop you from moving your foot too much
- Custom insoles or shoes for pain relief and arch support (orthotics)
- Less physical activity
If these therapies don’t ease your pain, or your symptoms get worse over 6 months, your doctor might consider surgery. It’s often recommended if your condition is past stage 2.
The surgery might include a combination of:
Talonavicular cuneiform arthrodesis. This procedure is done to ease your foot pain and restore some arch support.
Bone grafting. For this procedure, your doctor will take a piece of bone from your hips, legs, or ribs and use it to repair your damaged foot bones. In some cases, they might use bone from a donor.
There are other types of surgeries for this condition, such as joint fusion, but they are less common. You may need physical therapy before and after your surgery to help you recover.
What’s the Outlook?
Over-the-counter pain medications, custom shoes, and foot braces might help ease your pain, take any pressure or stress off your feet, and improve your quality of life. If these therapies don’t help, talk to your doctor to find out if surgery might be an option for you.
Show Sources
Mayo Clinic: “Avascular Necrosis (Osteonecrosis).”
Johns Hopkins Medicine: “Bone Grafting.”
Indian Journal of Musculoskeletal Radiology: “Mueller Weiss syndrome, a less elucidated and unusual cause of midfoot pain: A case report.”
World Journal of Orthopedics: “Müller-Weiss disease: Four case reports.”
Foot and Ankle Clinics: “Management of Muller-Weiss Disease.”
Foot and Ankle Online Journal: “Case study of idiopathic degeneration of the talonavicular joint.”
American Journal of Roentgenology: “Imaging of Mueller-Weiss Syndrome: A Review of Clinical Presentations and Imaging Spectrum.”
Mallory-Weiss Tear
Severe and prolonged vomiting can result in tears in the lining of the esophagus. The esophagus is the tube that connects your throat to your stomach.
Mallory-Weiss syndrome (MWS) is a condition marked by a tear in the mucous membrane, or inner lining, where the esophagus meets the stomach.
Most tears heal within 72 hours without treatment, but Mallory-Weiss tears can cause significant bleeding. Depending on the severity of the tear, surgery may be necessary to repair the damage.
The most common cause of MWS is severe or prolonged vomiting. While this type of vomiting can occur with stomach illness, it also frequently occurs due to chronic alcohol use or bulimia.
Other conditions can result in a tear of the esophagus as well. These include:
- trauma to the chest or abdomen
- severe or prolonged hiccups
- intense coughing
- heavy lifting or straining
- gastritis, which is an inflammation of the lining of the stomach
- hiatal hernia, which occurs when part of your stomach pushes through part of your diaphragm
- convulsions
Receiving cardiopulmonary resuscitation (CPR) can also lead to a tear of the esophagus.
MWS is more common in males than in females. It occurs more often in people with alcoholism. According to the National Organization for Rare Disorders, people between the ages of 40 and 60 are more likely to develop this condition. However, there are cases of Mallory-Weiss tears in children and young adults.
There are a few predisposing factors that can put you at risk of Mallory-Weiss tears. These can include:
- heavy alcohol consumption
- bulimia nervosa diagnosis
- persistent acid reflux
- severe vomiting
Having a hiatal hernia is currently up for debate as to whether it’s a risk factor for Mallory-Weiss tears. While many who have a diagnosis of MWS have reported having hernias, it’s still unclear whether there’s a proven link.
MWS doesn’t always produce symptoms. This is more common in mild cases when tears of the esophagus produce only a small amount of bleeding and heal quickly without treatment.
In most cases, however, symptoms will develop. These may include:
- abdominal pain
- vomiting up blood, which is called hematemesis
- involuntary retching
- bloody or black stools
Vomiting blood
Blood in the vomit will usually be dark and clotted and may look like coffee grounds. Occasionally it can be red, which indicates it’s fresh.
Blood that appears in the stool will be dark and look like tar, unless you have a large bleed, in which case it will be red.
If you have these symptoms, seek immediate emergency care. In some cases, blood loss from MWS can be substantial and life threatening.
There are other health problems that may produce similar symptoms.
Symptoms associated with MWS may also occur with the following disorders:
- Zollinger-Ellison syndrome, which is a rare disorder in which small tumors create excess stomach acids that lead to chronic ulcers
- chronic erosive gastritis, which is inflammation of the stomach lining that causes ulcer-like lesions
- perforation of the esophagus
- peptic ulcer
- Boerhaave’s syndrome, which is a rupture of the esophagus due to vomiting
It’s worth noting that MWS is a rare condition, and can only be diagnosed by a doctor. If you exhibit symptoms it’s important to see your physician immediately in order to get a proper diagnosis.
Your doctor will ask you about any medical issues, including daily alcohol intake and recent illnesses, to identify the underlying cause of your symptoms.
If your symptoms indicate active bleeding in the esophagus, your doctor may do what’s called an esophagogastroduodenoscopy (EGD).
You’ll need to take a sedative and a painkiller to prevent discomfort during this procedure. Your doctor will insert a small, flexible tube with a camera attached to it, called an endoscope, down your esophagus and into the stomach. This can help your doctor see your esophagus and identify the location of the tear.
Your doctor will likely also order a complete blood count (CBC) to confirm the number of red blood cells. Your red blood cell count may be low if you have bleeding in the esophagus.
Your doctor will be able to determine if you have MWS based on the findings from these tests.
According to the National Organization for Rare Disorders, the bleeding that results from tears in the esophagus will stop on its own in about 80 to 90 percent of MWS cases.
Healing typically occurs in a few days and doesn’t require treatment. But if the bleeding doesn’t stop, you may need one of the following treatments.
Endoscopic therapy
You may need endoscopic therapy if the bleeding doesn’t stop on its own. The doctor performing the EGD can do this therapy. Endoscopic options include:
- injection therapy, or sclerotherapy, which delivers medication to the tear to close off the blood vessel and stop the bleeding
- coagulation therapy, which delivers heat to seal off the torn vessel
Extensive blood loss may require the use of transfusions to replace lost blood.
Surgical and other options
Sometimes, endoscopic therapy isn’t enough to stop the bleeding. So doctors use other ways of stopping it, such as laparoscopic surgery to sew the tear.
If you can’t undergo surgery, your doctor may use arteriography to identify the bleeding vessel and plug it to stop the bleeding.
Medication
Medications to reduce stomach acid production, such as famotidine (Pepcid) or lansoprazole (Prevacid), may also be necessary. However, the effectiveness of these medications is still under debate.